What is Ecchymosis? Definition
The blood vessels (capillaries) under the skin are very minute. When they rupture, blood can escape from the vessels to the surrounding tissues. Rupture of the blood vessels can normally happen with or without trauma.
Under normal conditions the broken vessels are immediately sealed by platelets which come together and forming a plug. Further it is strengthened by fibrin deposits formed through a series of chemical reactions which is known as Coagulation cascade. [18] When the blood leaks into the subcutaneous space, it would be visible over the skin as a colour change, with or without swelling.
Origin: Greek [1]
Pronunciation: ‘eki-mosis’ [8]
For reimbursement purposes Spontaneous ecchymosis is coded under ICD-10-CM Diagnosis Code- 23.3 [17]
Skin – Layers
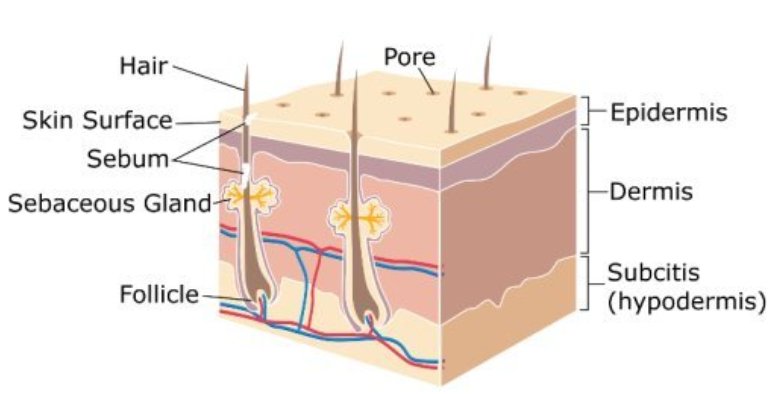
Image 1: Layers of skin- Epidermis, dermis and hypodermis (Sub-cutaneuos layer). The blood vessels can be noted in hypodermis and dermis layers.
Picture Reference: drebru.com
A purple red or blue discoloration occurring on the skin spontaneously, with or without trauma and measuring more than 1cm (10mm) is Ecchymosis. [2]
The term ecchymosis is sometimes confused with bruise/contusion, haematoma, purpura and petechiae.
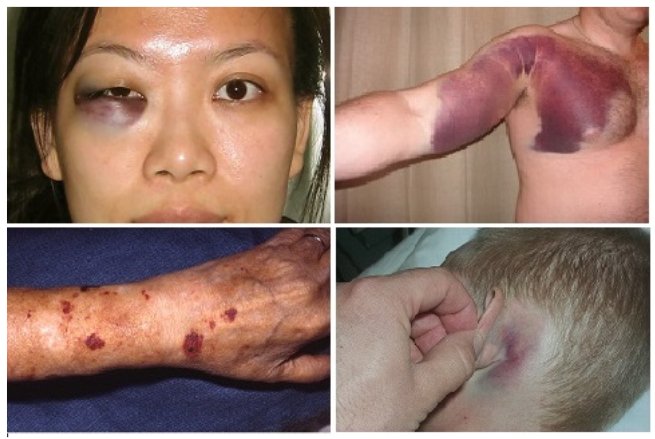
Image 2: Ecchymoses at various sites. Clockwise from top left (a) Periorbital ecchymosis (b) Upper arm and chest wall ecchymosis (c) Postauricular ecchymosis (d) Forearm ecchymosis
picture Ref: drugsdetails.com
What is Bruise/ Contusion?
It is ecchymosis that occurs due to trauma. It is better to remember as ‘All Bruises are Ecchymosis, but all ecchymoses (plural form of ecchymosis) are not bruises’.
What is the difference between a Hematoma and Ecchymosis?
Hematomas are also leakage of blood from the blood vessels. This may occur under the skin or near to any organs.
Ecchymosis occurs only under the skin and is flat when felt with fingers. Secondly, hematomas are formed by clotted blood which can raise the level of the skin or the surface of the organ. [9, 10]
Ecchymosis Vs Petechiae Vs Purpura (pictures)
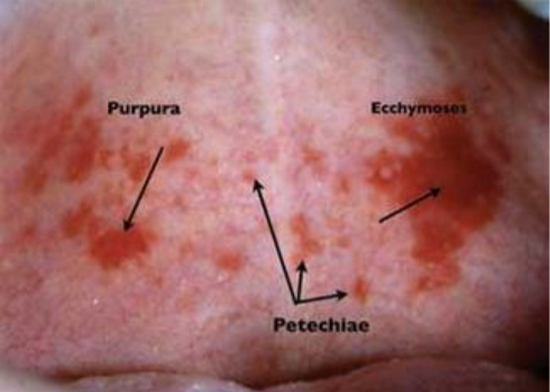
Image 3: Difference between Purpura, petechiae and Ecchymosis can be appreciated in this image.
picture source : rdhmag.com
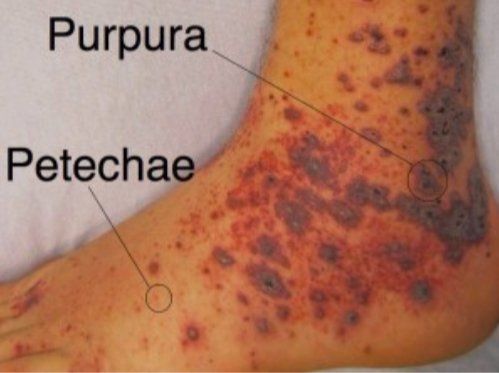
Image 4: The image shows petechiae and purpura lesions on the foot and the ankle.
picture source : emdocs.net [11]
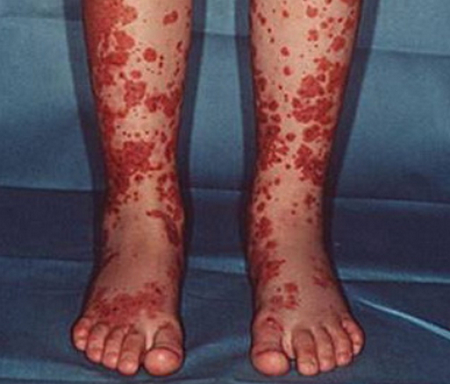
Image 5 : Henoch Schonlein Purpura
photo source : drmed.cn
Petechiae and Purpura occurs due to leakage of blood from the blood vessels to the surrounding tissues. This is same in the case of ecchymosis. The difference can be noted in their size. Petechiae are very small and may measure up to 3mm, whereas, purpura measures between 3mm and 1cm (10mm).
More than 10 mm, they are called as ecchymosis. None of the three blanch with application of pressure. In cases of petechiae or purpura due to vasculitis or infection, they may be palpable. [11, 16]
Causes of Ecchymosis
Disorders of blood vessels and surrounding tissue
- Physical abuse- The injuries will reflect the shape of objects with which injuries were caused. History given by the patient or relatives may not reflect abuse.[18, 19, 20]
- Vitamin C deficiency- The diet history may show deficiency of vitamin C intake. Clinically gum abnormalities or impaired wound healing might be observed.
- Idiopathic- Most of the cases may present with an unknown cause. This is most commonly seen among females who present with ecchymosis on their upper arms and legs.
- Amyloidosis- With different types of amyloidosis, the symptoms may vary. Usually they may present with generalised body swelling, organ dysfunction, nervous system dysfunction, enlarged heart, pain in the abdomen, foot or hands etc.
- Ehlers- Danlos syndrome– It is a genetic disorder characterized by hyper-elastic skin, hyper-mobile joints, translucent skin and dilatation of blood vessels.
- Hereditary hemorrhagic telengectasia – A hereditary condition which presents with anaemia, chest pain, shortness of breath, gastro-intestinal bleeding etc.[22]
- Marfans syndrome – Genetic disorder that affects the connective tissues. It is characterized by tall and thin stature with long arms and fingers, mitral valve prolapse, high arched palate, crowded teeth, extreme near sightedness, flat foot etc. [21]
- Osteogenesis imperfecta – This is also a genetic disorder which affects the collagen synthesis. The suffering patient may present with normal or short stature, easily fractured bones, blue sclera, dental problems, spinal curvatures and other abnormalities of collagen disease. [23]
Platelet abnormalities
Drugs
- Anti-coagulants – Heparin, Warfarin
- Non-steroidal anti-inflammatory drugs (NSAIDS) – Naproxen, Ibuprofen
- Anti-platelet drugs – Aspirin, Clopidogrel
- Corticosteroids – Prednisone, Hydrocortisone. Patients on long term use of these drugs may present with ecchymosis. This is mostly due to collagen absence, fragmentation or degeneration that occurs with corticosteroid use [35].
- Anti-cancer drugs
- Antibiotics
- Antidepressants
- Quinidine
- Alcohol – Liver cirrhosis can occur in chronic alcoholism which leads to liver dysfunction. This leads to a decrease in clotting factors.
Herbs and supplements
- Garlic
- Fish oil
- Ginko
- Vitamin E
- Von Willebrand disease – Von Willebrand factor is an important component of the coagulation cascade. The deficiency or defectiveness of the factor affects the blood clotting and may present as nose bleeding, gum bleeding, excessive bleeding from cuts etc.[24]
- Leukemia – When there is a cancer of blood forming cells, the normal cells are decreased. This can result is easy bruising weight loss, loss of appetite etc. [25]
- Lymphoma – The immune system cells such as lymphocytes when become cancerous, are called as lymphoma. Weight loss associated with chills and rigors and swollen lymph nodes may be the presentation in such a case. [26]
- Gaucher disease – An autosomal recessive disorder that affects the metabolism of fat. They can be characterised by hepatosplenomegaly (liver and spleen are enlarged), weak bones and bleeding disorders. [27]
- Wiskott Aldrich Syndrome – It is a X chromosome linked recessive disorder in which there is a decreased platelet count leading to bleeding disorder. It may also show with eczema and recurrent infections. [28]
Coagulation disorders
- Liver disease- Coagulation factor deficiency can occur due to the liver disease.
- Vitamin K deficiency- Vitamin K dependant clotting factors will be absent or decreased in Vitamin K deficiency. This can result in bleeding disorder.
- Coagulation factor deficiency- The deficiency may occur due to many causes such as liver disease. Usually there can be a family history present. The coagulation factors deficiency is characterized by bleeding from various sites including nose, gums, wounds, skin etc.
Ecchymosis – Different signs associated
It is very interesting to know that ecchymosis in different regions are given different names.
- Raccoon Eye sign – Ecchymosis which is common with eyeball injury or trauma results in periorbital ecchymosis (Ecchymosis surrounding the eye). [30, 31]
- Battle sign – In cases of basilar skull fracture, ecchymosis is commonly seen behind the ear, which is also known as Retroauricular/ mastoid ecchymosis.[32, 33]
- Cullen sign – Ecchymosis surrounding the umbilicus. [32]
- Grey turner sign – In some cases of acute pancreatitis, ecchymosis may be seen on lateral side of abdomen.[32]
- Crescent sign – The bony projections on each side of the ankles (Malleoli), may show ecchymosis.[34]
- Stabler sign – The inguinal-pubic area showing ecchymosis. [34]
- Fox sign – Outer side of upper thigh showing ecchymosis.[34]
- Blue scrotum sign of Bryant – Scrotal ecchymosis.[34]
How to diagnose the cause of Ecchymosis?
In cases of ecchymosis, a detailed history, including family and medical history is of utmost importance. Further, physical examination with emphasis on relevant suspected causes should be undertaken.
In general, a complete blood count (CBC), prothrombin time (PT) and activated partial thromboplastin time (PTT) should be done. [18] Other detailed investigations will vary from person to person on the basis of suspected cause. The tests could be done to confirm a diagnosis or to exclude some others.
Treatment for Ecchymosis
The treatment is based on the cause of ecchymosis. Usually they disappear without any treatment. The underlying cause once diagnosed, it is the one which would require a treatment, rather than ecchymosis.
References:
- http://www.pediatrics.wisc.edu/education/derm/tutb/85.html
- https://en.wikipedia.org/wiki/Ecchymosis
- http://mddk.com/ecchymosis.html
- https://en.wikipedia.org/wiki/Purpura
- http://www.nlm.nih.gov/medlineplus/ency/article/003235.htm
- https://commons.wikimedia.org/wiki/File:Purpura_Schonlein_Henoch.JPG
- http://www.medicinenet.com/script/main/art.asp?articlekey=3180
- https://medical-dictionary.thefreedictionary.com/ecchymosis
- http://www.pharmadhoc.com/uploads/3/2/7/4/3274790/2.bruise_and_contusion_convention.pdf
- http://wikidiff.com/hematoma/ecchymosis
- Murphy-Lavoie H and Leigh LeGros T. March 2010. emedmag.com
- http://drebru.com/unt/articles/yagli-cilt-articles/trbeauty-questions-myths-debunked-pores-skinencildinizdeki-porlar-ve-soylenceler-guzellik-sorulari/
- https://drugsdetails.com/ecchymosis-definition-types-symptoms-causes-diet-and-treatments-pictures/
- http://www.rdhmag.com/articles/print/volume-29/issue-4/columns/oral-exams/petechiae-ecchymoses-or-purpura.html
- http://www.drmed.cn/Henoch-Schonlein-purpura
- http://www.emdocs.net/9009-2/
- http://www.icd10data.com/ICD10CM/Codes/R00-R99/R20-R23/R23-/R23.3
- https://www.uptodate.com/contents/easy-bruising?source=contentShare&csi=bf62baae-5328-4f4d-87ee-3615eaef2a8a
- https://www.uptodate.com/contents/image?imageKey=PC%2F73534&topicKey=PC%2F16287&source=see_link&utdPopup=true
- https://www.uptodate.com/contents/image?imageKey=PC%2F67597&topicKey=PC%2F16287&source=see_link&utdPopup=true
- https://www.mayoclinic.org/diseases-conditions/marfan-syndrome/symptoms-causes/syc-20350782
- https://rarediseases.org/rare-diseases/hereditary-hemorrhagic-telangiectasia/
- http://www.childrenshospital.org/conditions-and-treatments/conditions/osteogenesis-imperfecta/symptoms-and-causes
- https://www.hemophilia.org/Bleeding-Disorders/Types-of-Bleeding-Disorders/Von-Willebrand-Disease
- https://www.medicinenet.com/leukemia/article.htm
- https://www.emedicinehealth.com/lymphoma/page4_em.htm#what_are_lymphoma_symptoms_and_signs
- https://www.mayoclinic.org/diseases-conditions/gauchers-disease/symptoms-causes/syc-20355546
- https://emedicine.medscape.com/article/137015-overview
- James WD, Berger TG, Elston DM. Andrews’ Clinical Diseases of the Skin Clinical Dermatology 10th edition. Elsevier, Inc. 2006.
- Fleisher GR & Ludwig S. Textbook of Pediatric Emergency Medicine 6th edition. Lippincott Williams & Wilkins. 2010.
- Mackenzie W. A Practical Treatise on the Diseases of the Eye. Longman, Brown, Green and Longmans. 1854.
- Epperla N, Mazza JJ, Yale SH. Wisconsin Medical Journal Volume 114 Number 2. April 2015.
- Caroline NL. American Academy of Orthopedic Surgeons. Nancy Caroline’s Emergency Care in the Streets, Volume 2. Jones & Bartlett Learning. 2007.
- https://emedicalhub.com/ecchymosis/
- https://jamanetwork.com/journals/jamadermatology/article-abstract/527721


