What is Petechiae?
Definition : When small blood vessels (capillaries) break under the skin, they cause reddish, brownish or purplish spots over the skin, which resemble rashes (3). When the size of the spots is less than 3 mm, they are called as Petechiae (4).
It does not blanch when pressure is applied on it. Occasionally the petechiae may be palpable as in case of vasculitis (5).
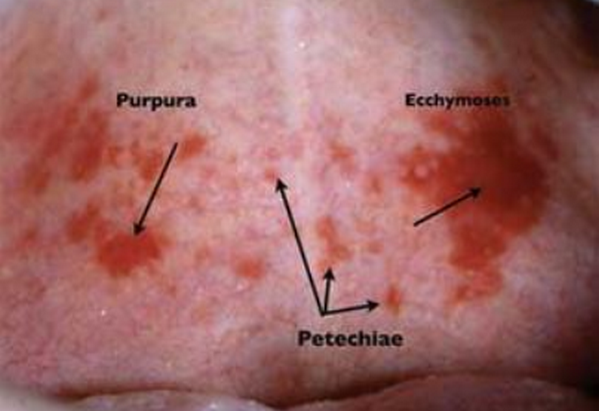
Picture 1: The image differentiates between Petechiae Vs ecchymosis Vs purpura.
Photo Source: pennnet.com
Origin & Pronunciation
- Origin- Italian (specks or freckles on face), Modern Latin [1]
- Pronunciation-
- Single- Petechia- pi-tee-kee-uh [2]
- Plural- Petechiae- pi-tee-kee-ee [2]
Layers of Skin
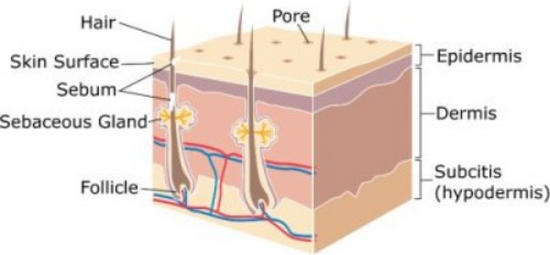
Picture 2 : Layers of skin- Hypodermis (Sub-cutaneuos layer), dermis and epidermis can be noted in this picture.
Image Source: i0.wp.com
What is Purpura?
Purpura is also due to leakage of blood from broken capillaries into the surrounding tissues. The size of purpura is slightly higher than that of petechiae. The spots on the skin measure from 3 mm to 1 cm (6).
Causes
Why would blood leak from blood vessels? This can occur due to the any of the reasons as given below. Petechiae are mostly seen with blood vessel abnormalities than clotting or coagulation abnormalities (7).
Blood vessel abnormalities
- Trauma to blood vessels- When there are minor injuries to the blood vessels, this leads to blood leakage.
- Infections- Certain bacterial and viral infections can lead to petechiae. Eg: Rocky mountain spotted fever, CMV infection, parvovirus infection, Scarlet fever etc.
- Vitamin C deficiency- Vitamin C is an important nutrient required for synthesis of collagen which in turn is required for skin, cartilage, bones and blood vessels. Hence deficiency of vitamin C can lead to blood vessel walls becoming weak and further leading to bleeding disorders.
- Ehlers-Danlos syndrome- This is an inherited disorder resulting in defective collagen synthesis. As described earlier, collagen defect can lead to blood vessels being weak.
- Pigmented purpuric dermatoses- This occurs due to inflammation of small blood vessels such as capillaries. Due to the disorder there can be petechiae or purpura along with pigmentation on the skin.
Blood clotting or coagulation abnormalities
- Decrease in platelet counts (Thrombocytopenia)
- Clotting factor deficiencies – Von Willebrand disease, Hemophilia, Vitamin K deficiency, Liver disease
- Disseminated intravascular coagulation.
Others
- Straining for prolonged duration as in case of child birth, weight lifting, crying etc(8).
- Drugs – Aspirin, Carbamazepine, indomethacin, morphine, naproxen, warfarin, heparin, cortisone, nitrofurantoin, penicillin etc.
| Platelet defects or deficiency | Clotting factor deficiencies | ||
| Petechiae |
Image 3: Petechiae over the mucosa of lips. |
Bleeding through nasal cavity, oral mucosa, and genitourinary tract is common. | Bleeding into joint spaces and muscles are uncommon. |
| Ecchymosis |
Image 4: Ecchymosis and petechiae seen over buccal mucosa in a case of idiopathic thrombocytopenic purpura.
Image 5: Battle sign seen in basilar skull fracture. It is also known as mastoid ecchymosis. |
Bleeding into the skin and mucous membranes can be seen usually as small, but may be a large area in severe states. | Can occur near to viscera and can lead to hematoma formation in the soft tissues. |
| Haemarthrosis |
Image 6: Haemarthrosis in the right knee of a patient suffering from haemophilia. |
Muco-cutaneous bleeding is very uncommon. | Haemarthrosis can be common in case of severe clotting factor deficiencies. |
| Bleeding due to small cuts or wounds | Commonly seen | Not that common. |
Table 1: Comparison between symptoms of various clotting abnormalities.(9)
How long do petechiae take to go away?
Petechiae appear due to particular reasons as explained above. The time taken for its complete disappearance varies from reason to reason. If it is due to minor causes, it may take a few days to few weeks for complete healing.
However, long standing causes can lead to petechiae persisting or reappearing for longer periods. This may be a few weeks to months.
Diagnosis
A complete physical examination along with a detailed history can help in pinpointing the diagnosis. Further, few laboratory tests are necessary to confirm the diagnosis(10).
- Complete blood count (picture)
- Peripheral smear
- Bleeding time and clotting time
- Prothrombin time (PT)
- INR (International Normalized Ratio)
- aPTT (Activated partial thromboplastin time)
- Specific clotting factor levels and activity
The above tests would help in a correct diagnosis of decreased count, bone marrow abnormalities, clotting factor deficiencies etc.
Treatment : How to get rid of petechiae
It would already be clear from above details that petechiae itself is not a disease but an expression/ symptom of an underlying condition. Hence, the treatment is also directed towards clearing the cause. If it is due to any medication, the respective medicine needs to be stopped for the petechiae to disappear.
Similarly, if the spots are due to infection, appropriate antibiotics may be required. Deficiencies of various factors such as vitamin C and K will have to be replaced. A platelet count fall mostly will need a correction with platelet transfusion(11,12,13,14,15).
Petechiae Pictures
Picture 7: Petechiae on the roof of mouth in a case of infectious mononucleosis.
Image Source: blogspot.com
Picture 8: Petechiae on leg of a patient.
Photo Source: healthline.com
Picture 9: Petechiae over the eyelids.
Image Source: bing.net
Picture 10: Petechiae on the foot.
Photo source: ytimg.com
Picture 11: Petechiae on the face in an elderly lady.
Image Source: consultant360.com
References:
- “petechia”. Online Etymology Dictionary. Douglas Harper, Historian. 20 Nov. 2017. <Dictionary.com http://www.dictionary.com/browse/petechia>.
- www.dictionary.com/browse/petechia
- www.mayoclinic.org/symptoms/petechiae/basics/definition/sym-20050724
- An Algorithmic Approach. Emergency Medicine Magazine. March 2010. emedmag.com
- emdocs.net/9009-2/
- Robbins basic pathology (8th ed.). Saunders/Elsevier. pp. 10–11
- www.uptodate.com/contents/evaluation-of-purpura-in-children
- www.mayoclinic.org/symptoms/petechiae/basics/causes/sym-20050724
- www.uptodate.com/contents/image?imageKey=HEME%2F77834&topicKey=HEME%2F1367&search=Clinical%20manifestations%20of%20bleeding%20disorders&rank=1~150&source=see_link
- A practical approach. Br J Haematol 2006; 133:221.
- en.wikipedia.org/wiki/Petechia
- www.mayoclinic.com/health/petechiae/MY01104
- www.nhlbi.nih.gov/health//dci/Diseases/thcp/thcp_signs.html
- symptom.healthline.com/symptomsearch?addterm=Petechiae
- www.dermatology.ucsf.edu/education_training/140.01ClinicalDermatology/MODULES%20UCSF/Petechia%20Purpura%20Vasculitis.pdf


