What is Bacteremia?
Bacteremia is the term which denotes the presence of bacteria in the blood. Whenever any kind of bacteria is detected in the blood, it is considered as the bacterial infection of the blood and is called as Bacteremia.
Based on the source of bacteria, Bacteremia is classified as Primary and Secondary bacteremia.
- When the bacteria are directly introduced into the body of a previously healthy individual through contaminated injections, catheters and other invasive procedures, it is known as Primary bacteremia.
- When the bacteria enter through a pre-existing breach of human tissue, like wounds in the skin, it is known as Secondary bacteremia. [1]
Based on the duration of the infection, bacteremia is classified as transient, periodic and persistent. Transient bacteremia is the presence of bacteria in the blood stream for few hours in which it is completely cleared off by the inherent immunity of a healthy person.
Periodic bacteremia is one in which the bacteria in blood stream survives until its source in the body is cured completely. This condition occurs in the presence of abscess or any other focus of infection in internal organs.
Persistent bacteremia occurs in long standing bacterial infections and infection of the blood vessels [2,3]
Pathophysiology of Bacteremia:
The bacteria which enter into the blood stream are often attacked by our immune system and cleared off. Those bacteria which escape this mechanism and the quantity which overwhelm the immune system, remains viable in the blood stream and cause bacteremia.
When the bacteremia become persistent, they reach major internal organs like heart, lungs and brain and form multiple foci of infection. Unless treated aggressively, the persistent bacteremia has a high mortality rate. [4,5]
Signs and Symptoms:
Transient bacteremia is mostly asymptomatic. Periodic bacteremia presents with nonspecific symptoms like fever, chills, rashes, nausea and vomiting and body pain. When the source of periodic bacteremia is not treated, it may lead to persistent fever, rapid breathing, delirium, hypotension and sepsis.
In permanent bacteremia, the symptoms are more severe including multifocal infection and sepsis, which may be fatal. When there is a focus of infection, the symptoms are specific to that organ. For example, neck stiffness and seizures in meningitis, respiratory distress in pneumonia, necrosis of limbs in cellulitis.
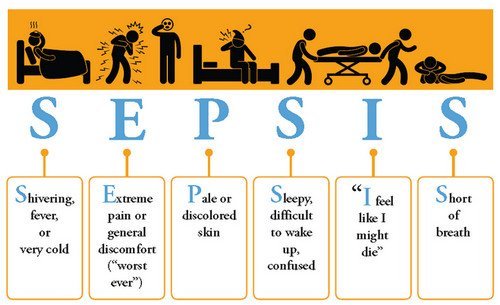
Image 1: symptoms of sepsis
Picture Source: www.biggiesboxers.com
Occult Bacteremia:
In some cases, a person remains symptomless and appears healthy, while the culture reveals presence of bacteria in the blood stream. Such a condition when the source of infection is obscure or the patient is asymptomatic, it is known as occult bacteremia.
It is a recognizable phenomenon in children while less documented in adults.
Although the occult bacteremia in adults is less documented, a recent study shows that the absolute number of adults with occult bacteaemia is same as that of children. While the cause of occult bacteaemia in adults is mainly due to infection in the kidneys, it is never the cause in children.
In contrast to the organisms isolated in children, the organism which is predominant in adult is Enterobacteriaceae. Thus, occult bacteremia should be suspected in adult patients also and the appropriate causative organism should be looked for. There are no standard criteria for occult bacteremia in adults similar to the Rochester criteria for children [6, 7]
Diagnosis of Bacteremia:
The diagnosis of bacteremia begins with a detailed history of the patient. Look out for all the symptoms of bacteremia and focus on organ specific symptoms to identify the source. Do a thorough physical examination for the signs of bacteraemia.
Any suspicion of bacteremia can be confirmed by the lab investigations given below :
- The current standard screening test for bacteremia is White blood cell (WBC) count. Generally, an increased WBC count denotes bacterial infection
- Absolute neutrophil count (ANC)
- Estimation of Procalcitonin level has high specificity in detection of bacteremia and is very useful for illnesses of short duration
- Blood culture is the commonly used diagnostic technique for bacteremia. The blood is collected in aseptic condition and is incubated in a culture medium that promotes the growth of bacteria. Ideally, two blood samples from different sites are cultured and positive in both cultures, confirm bacteraemia.
- Culture of urine, stool and cerebrospinal fluid
Pitt Bacteremia Score:
The severity of a patient with bacterial infection is assessed by the Pitt Bacteremia Score
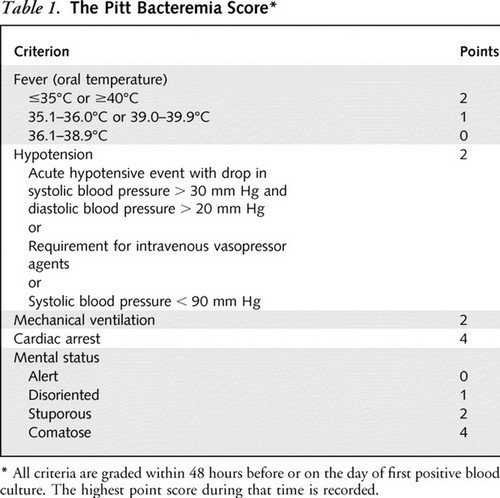
Picture 2: Pitt Bacteremia Score
Image Source: annals.org
Total score = SUM(points for all 5 parameters)
-
minimum score: 0
-
maximum score: 14
The higher the score, the more severe the bacteremia. [8]
Treatment
Low risk patients are treated as outpatients. Empirical treatment with broad spectrum antibiotics followed by organism – specific antibiotic after culture, is the mainstay of treatment.
High risk patients and those who are severely ill should be hospitalised and any focus of infection that acts as the source has to be cured completely to prevent recurrent and persistent bacteremia.
The duration of treatment for bacteremia caused by specific organisms is based on IDSA (Infectious Disease Society of America) recommendations. [9, 10]
Difference between Bacteremia and Septicemia
Bacteremia Vs Septicemia
As mentioned above, Bacteremia is the presence of bacteria in the blood stream. Septicemia or sepsis is the immune response of the body to the bacteria in blood stream. Sepsis is a syndrome comprising of various physico chemical reaction due to the inflammatory response against the infection.
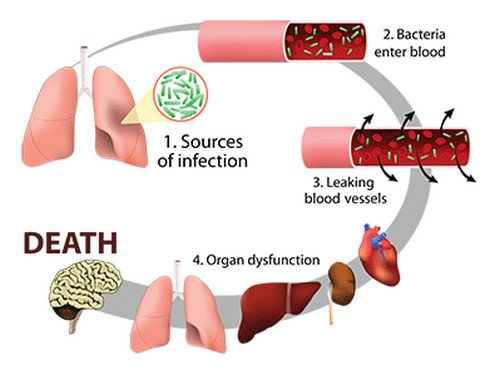 Image 3: Pathophysiology of sepsis
Image 3: Pathophysiology of sepsis
Picture Source: jeffreysterlingmd.files.wordpress.com
Although sepsis is viewed as the progression of bacteremia, only 30% cases of sepsis gets positive blood culture for bacteria. Thus the remaining 70% cases are septicemia without bacteremia. This condition occurs when there is a focus of infection in the internal organs like lungs which elicits the inflammatory response.
The signs and symptoms of persistent bacteremia constitute sepsis which may proceed to multi-organ failure, septic shock and death. Although all patients with bacteremia do not proceed to sepsis, they always have a risk of developing sepsis.
Therefore, appropriate antibiotic therapy is necessary to prevent the progression of bacteremia to sepsis. [11]
References:
- Pathophysiology of Infectious Diseases, ocw.tufts.edu. Retrieved 2016-12-07
- Harrison’s Principles of Internal Medicine, 19e.
- Seifert, Harald (2009-05-15). 48 (Supplement 4): S238–S245. ISSN 1058-4838. PMID 19374579. doi:10.1086/598188
- Scott, Michael C. (2017-02-01). “Defining and Diagnosing Sepsis”. Emergency Medicine Clinics of North America. 35 (1): 1–9. ISSN 1558-0539. PMID 27908326. doi:10.1016/j.emc.2016.08.002.
- Hall, Keri K.; Lyman, Jason A. (2016-12-16). 19 (4): 788–802. ISSN 0893-8512. PMC 1592696 . PMID 17041144. doi:10.1128/CMR.00062-05.
- https://emedicine.medscape.com/article/967600-overview
- https://academic.oup.com/cid/article-pdf/32/4/559/1259275/32-4-559.pdf
- Paterson DL, Ko W-C, et al. Ann Intern Med. 2004; 140: 26-32.
- Liu, Catherine – Clinical Infectious Diseases. doi:10.1093/cid/ciq146
- American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: Crit Care Med. 1992;20(6):864
- Wacker, C; Prkno, A; Brunkhorst, FM; Schlattmann, P (May 2013). 13 (5): 426–35. PMID 23375419. doi:10.1016/S1473-3099(12)70323-7. Archived from the original on 2017-09-06


