What is Sepsis and Septicemia?
Definitions: Septicemia in simple terms can be said as infection in blood. This is the reason why it has been used with interchangeable terms such as ‘Blood Poisoning’, ‘Bacteremia’ and ‘Sepsis’. The infection in blood can be due to the organism itself being in the blood or may be due to products (toxins or enzymes) of organism being in the blood.
In fact it is important to know that the terms such as ‘blood poisoning’, ‘sepsis’ and ‘bacteremia’ are different from each other. In medical terminology, we do not use the term blood poisoning. It may have been used by doctors to convey to non-medical personnel regarding the condition or between non-medical personnel.(1, 3, 4, 5, 6)
ICD 10 code for Sepsis and Septicemia – A41.9

Septicemia Vs Bacteremia
In a normal scenario, there will be no bacteria in the blood. This is because our immune system clears it immediately if it comes. When bacteria are present in the blood, then it is called as bacteremia. It is not necessary that bacteria have to be in blood for an infection in blood to occur.
Even bacterial products can cause infection. Similarly it is not necessary that an infection should occur when bacteria enters the blood (1, 3, 4, 5, 6).
Conversely, septicemia is when an infection occurs in the blood. This may or may not be due to bacteremia. Further, septicemia can also be caused by other organisms such as fungus.
Septicemia Vs Sepsis
Sepsis is actually a clinical syndrome with a wide range of abnormalities such as biochemical and physiological conditions that occurs due to a dysregulated immune response of our body to an infection.
The definition of sepsis had changed several times over the last few years. Please remember that, some experts consider its definition different from the one given above.
But, in general it is known that there can be widespread abnormalities in the body systems, which may affect different organs or organ systems and can result in failure of organs (Multiple organ dysfunction syndrome – MODS) and death. Severity of sepsis can range from septicemia, bacteremia, sepsis and septic shock to MODS and death.
In fact, sepsis is the better word to be used to describe the conditions related to infection of blood and its complications, as it is better defined than the others (1, 2).
Prevention, early diagnosis and treatment at the earliest possible occasion help to prevent the complications and problems that may arise due to sepsis.
Commonly used terms
In relation to septicemia, it is very common for people to use the term with the organism that causes the condition, or with the location the infection is or maybe with the condition itself. Few examples can be seen below(1, 3, 4, 5, 6).
- Gram negative septicemia – Bacteria are classified based on their staining properties. They are classified as gram negative and gram positive bacteria. When a septicemia is due to a gram negative organism, then it can be called as gram negative septicemia.
- Gram positive septicemia – Gram positive organism causing septicemia.
- Meningococcal septicemia – Meningococcus is a bacterium that can cause meningitis. It can cause septicemia.
- Puerperal septicemia – Infection in blood during the period of child birth.
- Neonatal septicemia – Septicemia in a neonate
- Wound septicemia – Septicemia that originates from a wound infection.
- MRSA septicemia – Methicillin resistant Staphylococcus aureus can cause septicemia.
How do you get Sepsis? (Pathophysiology of sepsis)
When an infective organism enters the blood, our body recognizes it and tries to neutralize the infection. This is done by certain cells of our system (macrophages and neutrophils) by either phagocytosing (eating) them or neutralizing it by release of chemicals. This is usually limited to the site of infection. On occasions, the body reaction goes uncontrolled and spreads to different regions through blood circulation (1, 7).
The origin of the reaction can be an infective source (organism, toxins of organisms, enzymes of organisms etc) or a non-infective source. When a non-infective condition such as trauma, pancreatitis etc results in such a reaction, then it is called a Systemic Inflammatory response Syndrome (SIRS).
The uncontrolled and unregulated immune response occurring thus is termed as sepsis. Though the exact mechanism that causes the immune response is not known, it is suggested that various factors could lead to the state. The bacterial toxins, bacterial cell wall components, excess inflammatory mediators, complement system activation and genetic predisposition are all suggested factors for the same.
The immune response through various mechanisms, that are unclear till now, causes the cells of various organs to get damaged and die. When multiple cells start dying in various organs such as blood vessels, lungs, kidneys, liver etc, the organs themselves start to fail, resulting in hypotension (septic shock), multiple organ dysfunction syndrome- MODS, and finally death.
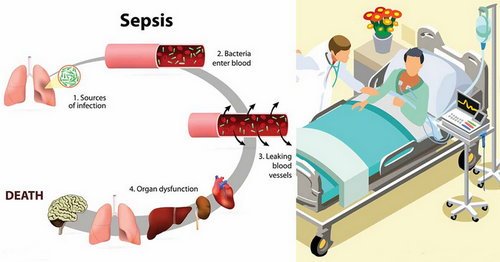
Picture 1: A picture demonstrating the broad pathophysiology of sepsis.
Image Source: media.mercola.com
Many a times, the question that is asked by common people is ‘Is sepsis contagious’? Sepsis as a condition is not contagious (1). But, when sepsis is due to an organism such as bacteria, virus or fungus, the organism can spread from person to person and cause various infections (1). For the said reason, it is very important to maintain sterile conditions while visiting a patient with sepsis (1).
Sepsis – Risk factors
Sepsis can occur in any individual. However, there are certain groups of individuals who are more prone to sepsis and its complications. The high risk groups to sepsis includes (1, 2, 8, 9)
- Age: People who are at extremes of age are more prone to sepsis. Advanced age (more than 65yrs) or too young are included in this group.
- Immunosuppression: Those who are under immunosuppressive medications (Anticancer medications, post organ transplant etc) or with immunosuppression due to disease condition (HIV infection) can be at higher risk to sepsis.
- Increased risk to infections due to diabetes or cancer
- Intensive care unit stay: Nosocomial infections are higher in intensive care and thus resulting in higher chances of sepsis.
- Patients with severe wounds or burns.
- Patients in whom spleen is removed. Spleen is an important organ in our body defense mechanism. Its removal can lead to frequent infections and sepsis.
- Genetic predisposition to sepsis.
- Patients with intravenous catheters, intra-urethral catheters and other invasive supportive devices.
Signs and Symptoms of Sepsis
It is very critical to identify and initiate treatment for anyone suspected to have sepsis. The continuum of sepsis in its early phase can be represented by an infection or bacteremia. A ‘Quick Sequential Organ Failure Assessment Score’ (qSOFA score) helps in diagnosing early sepsis.
This is easy and immediate to identify the condition, considering that only three factors need to be assessed. An altered mental status, respiratory rate equal to or more than 22 per minute and Systolic blood pressure equal to or less than 100mm of Hg. If any two of these are positive, the person is considered to be in early sepsis(1, 2, 8, 9).
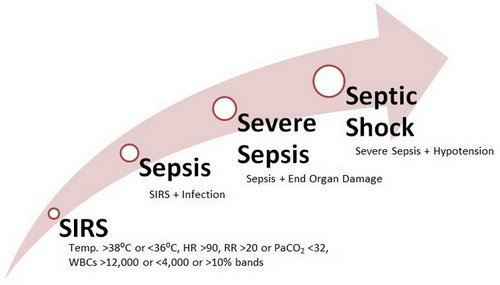
Picture 2: Stages of sepsis
Photo Source: i0.wp.com/ionhealthcarepulse.com
According to many experts sepsis can be divided into three stages. Many others do not consider this division.
1. Early sepsis
as discussed above is diagnosed by qSOFA score.
2. Severe Sepsis
Along with the symptoms of early sepsis, if someone has anyone of the following symptoms, then it is classified as severe sepsis. This is because the symptoms may indicate the start of any organ failing.
- Severely decreased urine output
- Decreased platelet count
- Difficulty in breathing
- Abdominal pain
- Sudden mental status changes
- Altered pumping by heart
3. Septic shock
Due to the sepsis, when the blood pressure falls very low and does not increase with intravenous fluids, along with signs and symptoms of severe sepsis, can be diagnosed as septic shock. The likelihood of septic shock necessitates the use vasopressors in sepsis.
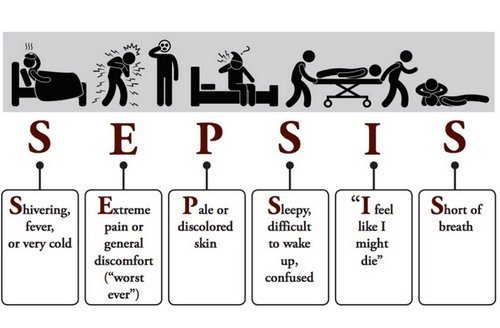
Picture 3: Clinical features of sepsis
Image Source: www.slate.com
There is no particular set of symptoms that appears in sepsis. Similarly the symptoms that appear in sepsis can resemble those in case of many other conditions. In general, the following symptoms should raise the suspicion or chances of sepsis in an individual.
- Infected wounds with abscess
- Cough with sputum indicating pneumonia
- Hypotension – Reduced blood pressure
- Hypothermia – Reduced body temperature
- Hyperthermia – Raised body temperature
- Tachycardia – Raised heart rate
- Tachypnoea – Raised respiratory rate
- Decreased capillary refill
- Cold clammy skin
- Cyanosis
- Reduced urine output
- Altered mental status
Diagnosis of Sepsis
The clinical diagnosis based on signs and symptoms helps in coming to an appropriate diagnosis of sepsis. Further, to confirm the diagnosis, various methods may be used to identify the source of infection. In general many of the following tests or investigations may be performed as it necessitates(2).
- Blood check for- WBC counts, blood sugar levels, plasma C- reactive protein, serum creatinine, INR, aPTT, platelet count, plasma bilirubin levels, serum electrolytes, serum lactate levels, plasma procalcitonin levels etc.
- Imaging techniques- CT scan, MRI scan and X-rays may be used to localize the infection source if suspected.
- Microbiology- Studies including microscopy, culture and sensitivity tests may be done for identifying any organisms present. But, it is not necessary for the diagnosis of sepsis.
Sepsis Treatment
The main stay in treatment of sepsis is antibiotic administration. This is because in most cases of sepsis due to infection, bacteria are the largest known cause. The patient is usually kept in intensive care under the care of critical care specialists (1, 3, 4, 5, 6).
Appropriate organ support might be required if impending organ failure occurs as dialysis in case of kidney failure.
Intravenous fluid administration along with vasopressors might be required to counter septic shock.
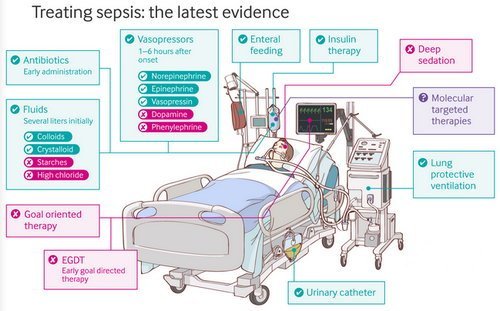
Picture 4: Treatment general outline in a case of sepsis
Image Source: sandpit.bmj.com
Complications of Sepsis
We have seen above that the various organs can get affected and may lead to their failure in sepsis. Other than organ failure, the condition may lead to tissue necrosis due to loss of blood supply leading to gangrene and tissue loss with amputation.
Sepsis has a high chance of resulting in death. Hence, early diagnosis and treatment is the way to better recovery (2, 10).
How can sepsis be prevented?
The complete reasons and pathophysiology of sepsis is still clearly unknown. Prevention of sepsis cannot be guaranteed. But certain steps such as treating any infections at the earliest and taking preventive steps against infections, does go a long way in prevention of sepsis.
Many serious infections have vaccines available that can be administered as a preventive step. Washing hands frequently and taking protective measures while visiting patients suffering from infections can also help (11).
References:
- medicinenet.com/sepsis/article.htm
- uptodate.com/contents/sepsis-syndromes-in-adults-epidemiology-definitions-clinical-presentation-diagnosis-and-prognosis
- Dellinger et al. “Surviving Sepsis Campaign Guide lines for Management of Severe Sepsis & Septic Shock.” Crit Care Med 32 (2004): 858-873.
- Kaplan, “Systemic Inflammatory Response Syndrome.” Medscape.com. Aug. 16, 2016. emedicine.medscape.com/article/168943-overview>.
- Surviving Sepsis Campaign. “Guidelines.” www.survivingsepsis.org/Guidelines/Pages/default.aspx>.
- United States. Centers for Disease Control and Prevention. “Sepsis Questions and Answers.” Sept. 16, 2016.www.cdc.gov/sepsis/basic/qa.html>.
- uptodate.com/contents/pathophysiology-of-sepsis
- mayoclinic.org/diseases-conditions/sepsis/symptoms-causes/syc-20351214
- emedicinehealth.com/sepsis_blood_infection/page2_em.htm#what_causes_sepsis
- www.mayoclinic.org/diseases-conditions/sepsis/diagnosis-treatment/drc-20351219
- www.uptodate.com/contents/sepsis-in-adults-the-basics?source=related_link